Two full weeks since my last post – holiday activities, don’t you know, starting on December 21 with a solstice party at the home of an eccentric friend. I see that my blog viewership has declined precipitously in the past week, so I’m happy that you all have better things to do at holiday time than to read about PSP. Don’t we all wish that the disease itself would take a few days off, too?
My re-emergent thought is about the famous “hummingbird sign.” On an MRI scan in the sagittal plane – that’s as if you sliced someone down the middle and looked at the cut surface – the brainstem sort of looks like a side view of a hummingbird.
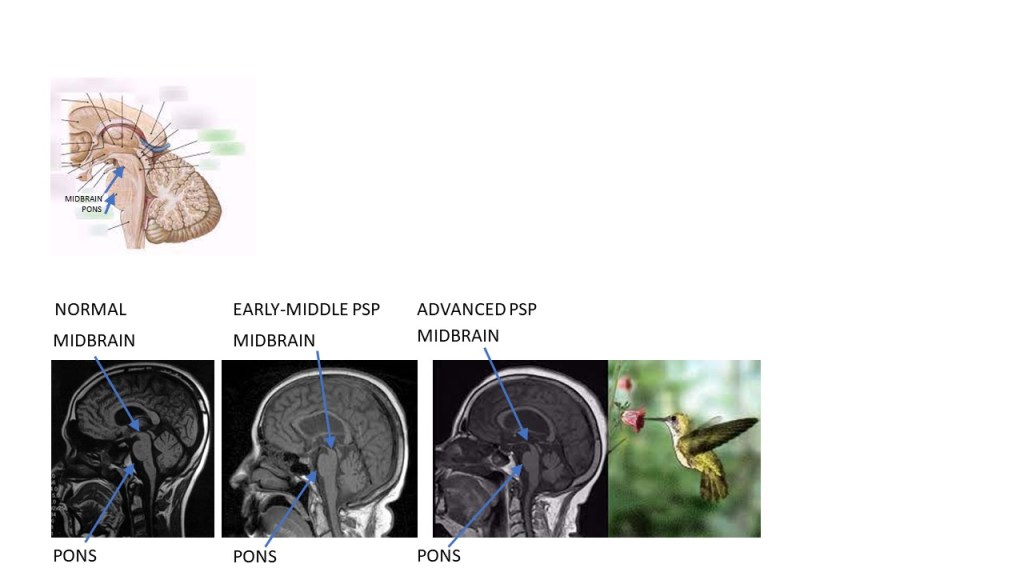
In the MRIs above, the nose is on the left. In the lower images, the arrows stop just short of the indicated structures so as not to obscure them. Note the progressively thinner, sleeker midbrain (the hummingbird’s head and beak) with retention of the plump pons (the belly, which is plumper than than that of a real hummingbird).
Now here’s the issue. The appearance of the hummingbird sign isn’t as closely related to PSP as has been implied by many. There are just too many false positives and false negatives.
The false positives mostly occur in people with normal-pressure hydrocephalus, a condition where the fluid-filled spaces in the brain (the “ventricles”) enlarge because of an obstruction in the re-absorption of the fluid into the bloodstream. This stretches the fibers adjacent to the ventricles, impairing control of gait, cognition and the bladder. It also presses down on the midbrain, producing the hummingbird sign. Then there are those individuals with corticobasal degeneration where the features resemble PSP (“CBS-PSP”). They can also have a hummingbird sign.
The false negatives occur in the first couple of years after the initial symptoms. They also occur if the MRI is mis-aligned on the brain or the head is a little rotated, producing an allegedly midline cut that’s actually a couple of millimeters to one side. That means that the thinnest part of the midbrain, which is in the midline, isn’t shown in the image.
You should also know that the hummingbird sign isn’t just about a thin midbrain. A normal pons is also part of the sign. That’s because in multiple system atrophy and a few rarer disorders, both the midbrain and pons become thinner. But in PSP, it’s mostly the midbrain that does so.
I think that in the next year or two, a test of the tau protein in spinal fluid, blood or a tiny punch biopsy of skin will provide a much more accurate diagnosis of PSP than the hummingbird sign. Soon thereafter we will probably have a PET technique that does the same. Then, clinical treatment trials can be accomplished faster because they won’t have to compensate for the statistical noise produced by participants with a false positive diagnosis. In fact, all sorts of research on PSP will become much more powerful if people without PSP can be excluded.
All my best for the New Year.