Now, this is progress. Novartis just yesterday announced in clinicaltrials.gov that its Phase 3 trial of NIO752 is ready to accept volunteers for screening. The name of the trial is PRESERVE. Good name. No, it’s not an acronym for anything.
So far, the company has only announced three trial sites (Rochester, MN; Englewood, CO; and Ulm, Germany) but dozens more will follow, with a total recruitment goal of 300. Here are some details of probable interest to potential volunteers:
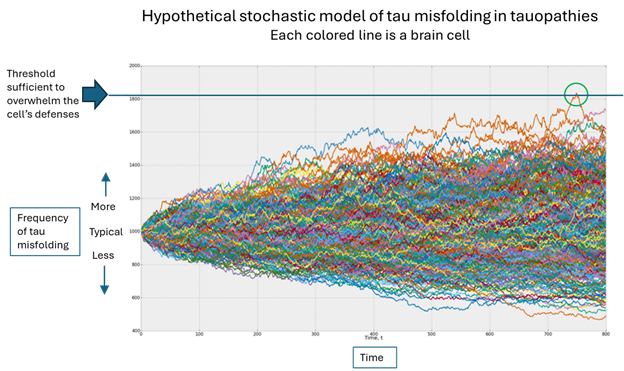
- The drug is an antisense oligonucleotide, which as you’ve learned from this blog, interferes with the brain cells’ ability to translate the RNA from a specific gene into its protein. In this case, the protein is tau, which lies at the heart of PSP.
- As a very large molecule, NIO752 cannot pass the blood-brain barrier, so it has to be injected directly into the cerebrospinal fluid in the lower spine, using the same procedure as a diagnostic spinal tap (lumbar puncture). This will be given every three months, assuming it follows the plan of the Phase 1 study.
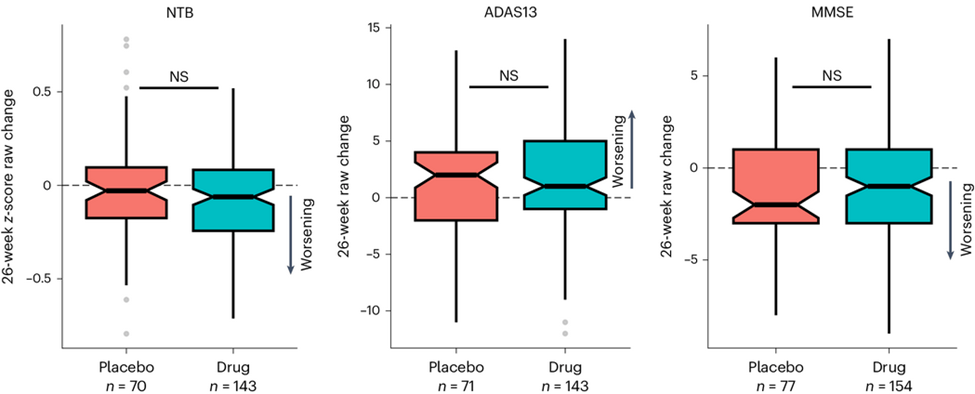
- A trial of the drug for safety in 45 people with PSP showed no important or permanent adverse effects from the procedure – just harmless and transient headaches or back pain in some. Some transient confusion or lethargy occurred in three of the 45 – an effect of the drug, not the injection procedure.
- The trial will enroll 300 participants overall, of whom 100 will be randomly chosen to receive a placebo injection. That treatment assignment will be double-blind — not revealed to participant or neurological staff until the whole trial is over.
- The duration of the double-blind period will be 72 weeks – about a year and a half. After that, all the patients will be offered the opportunity to continue receiving the drug at no cost, as long as it has not been found to be harmful, and as long as Novartis is still manufacturing it. That “open-label extension” program may end if and when the drug works and is on the market (let us pray).
Your big question right now should be this: Should I volunteer for the PSP Trial Platform (PTP) or PRESERVE? The scheduled start for PTP is next month (June 2026), and those sites will roll out gradually, just like the PRESERVE sites. So, in theory, there’s no overall difference in the timing, though a site near you might open for one study well before the other, or there may be an accessible site for one and not the other. All the PTP drugs and NIO752 are similarly and acceptably safe, in my view.
Right now, I’d say volunteer for PRESERVE, though by a slim margin. Two reasons, each minor:
- Like any large, complicated project requiring approvals from government, private companies and academic institutions, the PSP Trial Platform has been subject to unforeseen delays. (All major drug trials require collaboration among these three, but the PTP is more complicated than most.) In fact, the company sponsoring one of the three drugs planned for the PTP has still not finalized the arrangements, according to clinicaltrials.org. If that can’t be accomplished soon, the trial will start with only two drugs. So, a bird in the hand . . .
- The PRESERVE trial will have an open-label extension (see the caveats above), while the PTP has not yet decided on that, and it may differ across the different drugs. Without an open-label extension, someone completing the Phase 2 trial would have to wait until the Phase 3 is finished and the drug approved before gaining access to it. On the other hand, the FDA has been known to approve drugs for general use after only a Phase 2 if the need is great, and for PSP, it surely is. The PTP double-blind trials are 12 months long and the PRESERVE double-blind is nearly 18 months, so assuming both offer open-label extensions, someone on placebo in PRESERVE would have to wait six months longer to receive their active drug than someone in the PTP.
Yes, there are other drugs whose sponsors are optimistic that trials will start within the next year or so. Those include bepranemab (a monoclonal anti-tau antibody), GV1001 (an anti-inflammatory), ARV-102 (an enhancer of abnormal tau degradation) and TPN-101 (an inhibitor of a toxic protein called LINE-1). But the timelines there are just too uncertain for someone with PSP to consider right now.
Maybe the most important consideration is which drug is mostly likely to work. I honestly don’t know, and the Phase 1 data don’t answer that question. So that simplifies things a bit.
A difficult choice, I know, but a good problem to have.