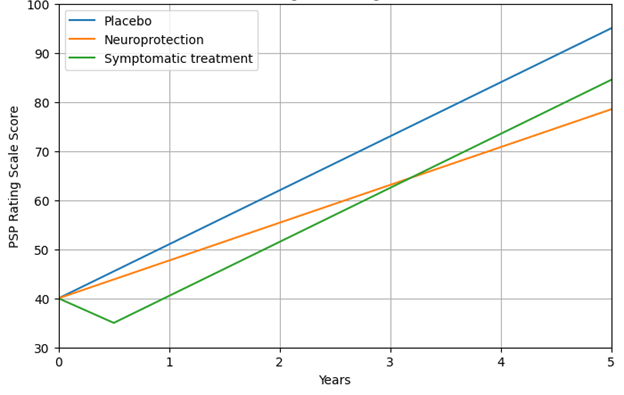The PSP Rating Scale has had quite the odyssey. I designed back in 1996 (30 years ago now!) to be used by neurologists or other clinicians working in movement disorders, and its specialized terminology reflects that. But some people with PSP or their caregivers have attempted to apply the scale themselves. That, and the continued importance of the scale in PSP research, prompt this update.
The scale and its tips/rules for its administration can be viewed and downloaded from the CurePSP website.
The PSPRS is intended mostly for use in routine clinical care and touches on all the common features of PSP. It’s designed to answer the question, “So, how am I doing, Doc?” on a 100-point scale, with zero being perfectly normal. It’s a measure of the severity of symptoms, not a set of diagnostic criteria. The most recent such criteria, if you’re interested, are available here. They’re also pretty technical.
The PSPRS includes 28 items, 22 rated 0-4 and six rated 0-2, divided into six sections. The first, “History” is rated via interview. The others, all requiring a neurological exam, are Mentation, Bulbar, Ocular Motor, Limb Motor, and Midline/Gait. (“Bulbar” means speech and swallowing, so named because the part of the brainstem where those things are controlled, the medulla oblongata, looks like a flower bulb or a fat scallion.)
The PSPRS scoring behaves thusly: The average person with PSP-Richardson syndrome, the most common PSP subtype, comprises about half of all patients) and worsens by an average of about 11 points per year, more slowly at the very start and end of their PSP journey. PSP-Parkinsonism, accounting for about 20% of all PSP, progresses about two-thirds as quickly. Most people entering clinical treatment trials (all with PSP-Richardson) have scores between 35 and 40, a figure heavily influenced by most trials’ rules that participants be in the early or middle disease stages.
Although I did not design it specifically for research use, the PSPRS became the world-wide standard measure in PSP research soon after its 2007 publication. However, the time required to administer it has prevented it from attaining much popularity for its original purpose as a routine tool in patient care. I can run through it in 10 minutes with a mildly affected patient, but physicians with less experience and patients with more complicated deficits require up to 20. With only 20 or 30 minutes scheduled by most medical practices for follow-up visits, you can see why the PSPRS has not attained popularity outside of research projects, where the visits include many more tests and require several hours.
Another issue with the PSPRS is that some of its 28 items relate more to the neurologist’s concept of what’s going on in the patient’s brain rather than directly to daily disability, which, after all, is the primary target of both routine care and research. Therefore, the FDA in the US has expressed a preference for its own 10-item version, which retains items only in the History, Bulbar and Midline/Gait sections and collapses some of the response options in most of the others. Naturally, the lesser precision of the “PSPRS-10” requires that the study recruit more patients to provide the statistical power to demonstrate a given degree of drug benefit and provides no information at all on eye/eyelid movement or cognitive/behavioral deficits. But researchers in Germany have applied a sophisticated statistical technique for drug trials called “item response theory” using all the study visits (typically about five over 12 months) rather than just the starting and ending visits. This allows the PSPRS-10 to exceed the original in its statistical power to detect a drug benefit despite the lesser supply of information from each visit.
The anti-sense oligonucleotide (ASO) trial, called “PRESERVE” from Novartis is the first to use the FDA’s PSPRS-10 as its primary outcome measure. The trial’s designers had little choice because as a Phase 3 trial, it is “pivotal” in the sense that it could make or break the drug in the eyes of the FDA. However, PRESERVE will add the original 28-item version to its secondary measures. They can be considered by the FDA to clarify a weak result in the primary measure. Its inclusion also makes life easier for future researchers seeking to integrate the study’s results into the large body of data available from previous drug trials.
Other abridged versions of the PSPRS-28 to date are:
- A 14-item version omits the items less relevant to daily activities, with each remaining item rated 0-2. It performs as well as the original for PSP-Richardson but not for the other variants, according to a trial by a different set of researchers.
- A 15-item version, also a subset of the original, which uses the results of the unsuccessful PASSPORT trial to omit items less related to daily activities as well as statistically redundant items and response choices. It offers better statistical power than the original or any of its other modified versions and is being used as the primary outcome measure in the PSP Trial Platform. The PTP can defy the FDA’s recommendation to use its 10-item version because those are only Phase 2 trials, not the Phase 3 pivotal trials that the FDA uses to decide on a drug’s final approval.
- 21- and 24-item versions omitting PSPRS-28 items problematic for tele-health administration. These have not yet reached widespread adoption for either routine practice or research, but they have excellent potential for use in pandemics or for patients with difficulty traveling to a neurologist for reasons of disability or distance. The only potential problem is wrangling the software.
None of the PSPRS versions allows reliable administration by the patient or caregiver, but the Cortico-basal Ganglia Functional Scale (CBFS) does so. In fact, it’s designed for use online or in the neurologist’s waiting room, with no instructions needed beyond what’s on the form. Despite its name, it has been validated for PSP as well as for corticobasal syndrome. So, if you want to rate yourself at home, use the CBFS rather than any of the PSPRS versions, and coordinate with your neurologist so as to make best use of the results.
Despite all this, the original content and wording of the PSPRS-28 have never changed. I’ve only refined the instructions and tips published along with it.
Finally, a little perspective: Despite all this hard work on various rating scales, measuring atrophy of the brain’s frontal lob on MRI tracks progression of the disease better than any of them. One careful analysis found that a trial designed to detect a 50% slowing of progression using the PSPRS-28 would need 112 subjects (half on active drug, half on placebo) and only 72 using the MRI measure. Of course, the FDA would never accept such a measure in a pivotal trial, but at least one current, early-phase PSP trial is using MRI as its primary outcome measure.
I refer to the PSPRS-28 as my own work, but some of the credit belongs to my statistician colleague at Rutgers, Pamela Ohman-Strickland, PhD. I couldn’t have validated the scale without her. I know because I tried.
Disclosure: I (and Pam) have a financial interest in the PSPRS via a sharing policy at Rutgers University, which owns the copyright and licenses it to pharma companies for use in their drug trials. Rutgers imposes no fee for its use in regular patient care or in research by non-profit organizations such as universities.