I spent most of last week attending two virtual conferences. One was the semiannual investigators’ meeting of the Tau Consortium. That’s a group of a few dozen researchers funded by the Rainwater Charitable Foundation. Attendance is limited to funded researchers, their trainees, and invited guests from organizations that work with the RCF. I got in as a representative of CurePSP. They keep attendance private so that speakers will feel free to share their work long before publication without fear of plagiarism. The other was Tau 2022, a biannual conference sponsored by the Alzheimer’s Association, the Rainwater Charitable Foundation and CurePSP, with help from a few drug companies. Registration was open to the public and I was on its Steering Committee, again representing CurePSP. Both conferences were stuffed with cutting-edge work by some of the world’s top researchers. I’m working on summarizing for you, dear reader, some of the things that I’m allowed to share, and that will take a few more days.
Meanwhile, I saw a cool paper in a journal called Sensors. Paula Stępień, a biomedical engineer at Silesian University and colleagues from multiple other institutions in Poland created an app that analyzes a commonly used, pen-and-paper neuropsychological test called the Luria Alternating Series Test. The examiner draws a series of connected triangles (actually inverted V’s) and squares (without the bottom side) an inch or two at the left of a sheet of paper. The patient then has to continue the series the rest of the way. Here are examples for someone with PSP (top), PD (middle) and a healthy control. The examiner’s model is the first five figures on the left of each line:
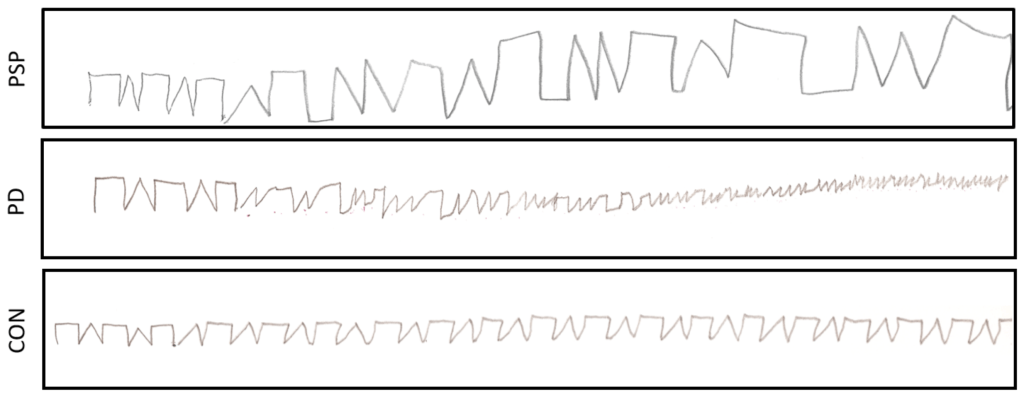
The algorithm looks at 35 possible error features and can label subjects as having PSP, PD or neither with 70.5% accuracy. While that’s not as good as MRI or a formal, in-person history and exam by a neurologist, it does have the advantage of being a lot easier and cheaper and can be performed remotely. Perhaps coupling it with some other tests similarly compatible with telemedicine could raise that accuracy figure. That could allow treatment trials to screen people with suspected PSP before bringing them in for the standard hours-long, in-person initial evaluation visit.
The article doesn’t mention how long the patients had PSP or PD or the severity of their outward signs, so perhaps the same diagnostic information could have been obtained by casual observation by video call. But like any diagnostic test, you first have to make sure it works in people with an existing diagnosis before you test it in those with early-stage or diagnostically equivocal symptoms.