Researchers led by Dr. Elena Vacchi of Lugano, Switzerland report new data on the utility of skin biopsies in the diagnosis of PSP and CBS. This diagnostic approach is further along for Parkinson’s, where the fibers of alpha-synuclein are not difficult to detect in the tiny nerves in skin. The same technique, but for tau, has not been particularly successful for PSP so far, but these researchers did more sophisticated molecular tests.
They recruited 11 patients with PSP and 4 with CBS, along with 31 with PD, 14 with MSA and 24 healthy controls. They obtained two cylindrical plugs of skin 3 mm in diameter from the back of the neck and another two from just above one ankle. They measured the amount of normal and abnormal tau protein and the forms of RNA encoding the most common abnormal tau forms found in PSP and CBD (the 2N4R isoform).
Comparing the group with PSP or CBS with the group with PD, there was a 90% sensitivity (i.e., the fraction of the patients with PSP or CBS whose biopsy showed an excess of abnormal tau) but only 69% specificity (the fraction of those without PSP or CBS with a normal result) and 0.812 AUC (see the note below). For the comparison of PSP/CBS versus MSA, the results were better: 90% sensitivity, 86% specificity and 0.900 AUC. I assume that that’s because of PD’s known tendency to have a little tau aggregation along with its alpha-synuclein, while that happens little in MSA. For some reason the comparison of PSP/CBS with healthy controls was only moderate, with an AUC of 0.774. The neck skin proved more informative than the ankle skin.
The authors point out that their patients’ diagnoses were not autopsy-confirmed. One solution might be to obtain the skin samples from deceased patients undergoing brain autopsy. They also point out that the pattern of excessive phosphorylation of tau, which is known to be critical to disease causation, was not considered at all in their otherwise-thorough lab procedures. So that might improve their results.
An interesting upshot is the authors’ observation that in PD and MSA, there was a reduction of nerve fibers in the skin, while this did not occur in PSP/CBS. Together with evidence from many other sources, this suggests to them that in PD and MSA, the disease starts in the peripheral tissue (i.e., in non-brain organs such as the skin) and spreads to the brain, while in PSP and CBD, the problem starts in the brain and spreads outwards.
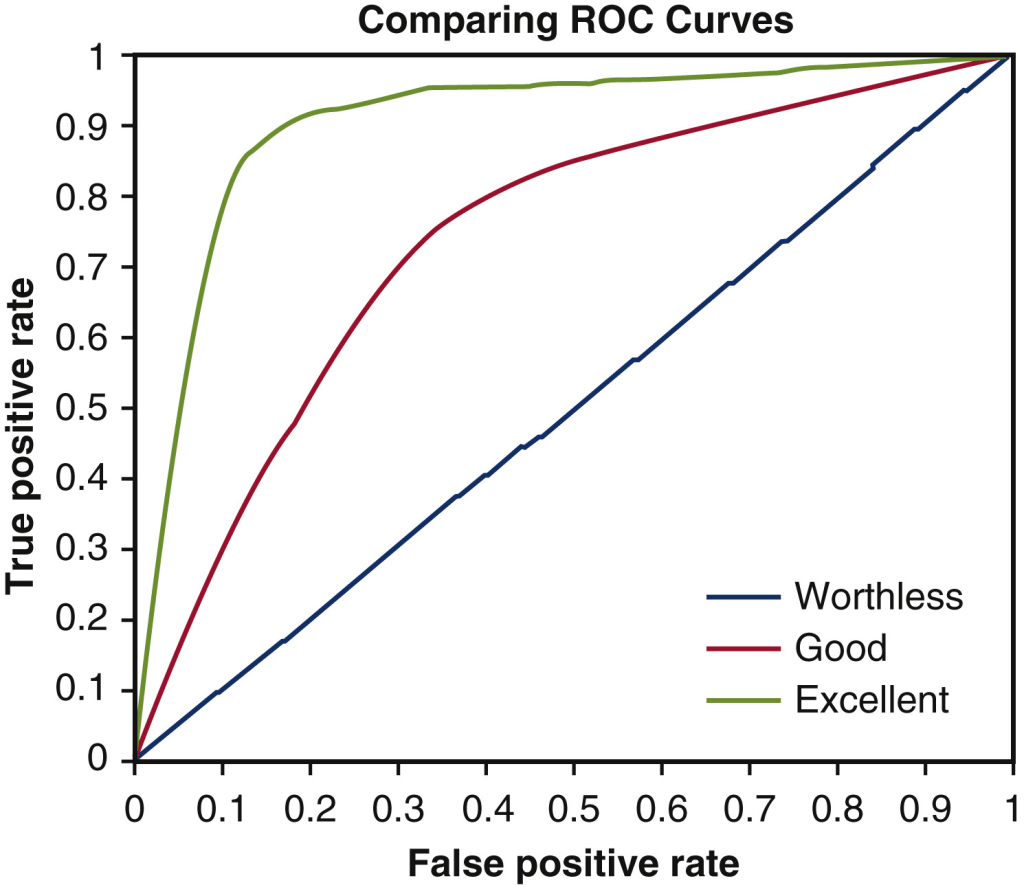
Note: Per Wikipedia, “A receiver operating characteristic curve, or ROC curve, is a graphical plot that illustrates the diagnostic ability of a binary classifier system as its discrimination threshold is varied.” In other words, how well does a simple positive/negative diagnostic test do in distinguishing true positives from true negatives? This allows you to optimize the definition of “positive” and “negative” test. The curve’s vertical axis is the sensitivity or the true positive rate (0 to 1.0) and the horizontal axis is 1 minus specificity or the false positive rate. The area under that curve (AUC) has a theoretical maximum of 1.0. Excellent diagnostic tests have an AUC of 0.90 or more, and moderate tests, 0.80 to 0.89. A coin flip’s AUC is 0.50.
Pingback: Imaging in the diagnosis of PSP | PSP Blog
You got it, pal.