In a reply to a commenter back in July 2022, I expressed pessimism about the neuroprotective potential of buntanetap, formerly known as posiphen. That drug is claimed to reduce genetic transcription of multiple neurodegeneration (NDD)-related proteins, including tau, at the messenger RNA (mRNA) level. I thought it unlikely that one drug could do that without impairing production of other proteins necessary to health and life.
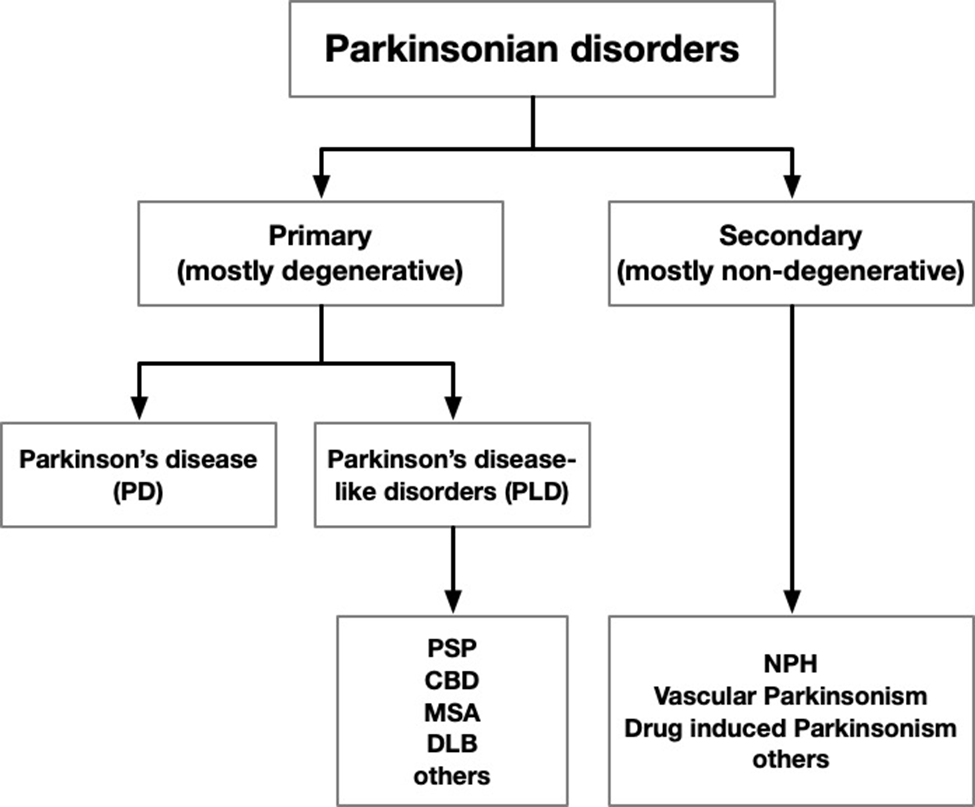
Later in the same year, 2022, a double-blind trial of buntanetap in Parkinson’s disease and Alzheimer’s disease was published. The N was small, with 54 participants with PD and 14 with AD. The treatment period was very short, only 25 days, which means that any result would reflect only symptomatic, not neuroprotective (disease-slowing), effects. That’s because the progression of PD and AD are too slow to be measured over only a 25-day period. However, the main purpose of the trial was to study safety and tolerability, not efficacy. The trial also checked spinal fluid levels of multiple proteins associated with the diseases – i.e., biomarkers.
The result were small but statistically significant improvement in some of the cognitive and motor measures in PD and some of cognitive measures in AD. Most of the biomarkers showed improvement, but none were statistically significant.
Some cell/molecular biology here, folks: The authors argue that previous attempts to treat NDDs by targeting only one protein at a time have failed because all the diseases actually include defects in multiple proteins. They point out that the mRNAs of multiple NDD-related proteins and iron-metabolizing proteins share a section called an iron-responsive element (IRE). But the mRNA for the iron-metabolizing proteins is very slightly different from that for the NDDs. IREs are not translated into any part of its parent protein, but they do regulate that protein’s production by the ribosomes: When the level of iron in the cell is too high, the IRE prevents the ribosomes from making the protein. The butanetap molecule binds to a specific part of the IRE, mimicking a high-iron effect. Luckily, the drug does not bind to mRNA of actual iron-metabolizing proteins – only to that of NDD-related proteins.
So, if you skipped that nerd interlude, the executive summary is that there’s a good scientific rationale for why buntanetap could work.
But there are some potential issues with the 2022 clinical trial:
- Many of the patients experienced minor side effects such as headache, rash or muscle spasms. This could have impaired the blinding scheme and produced a placebo effect. That issue could have been addressed by asking the patients at study’s end, before the randomization assignments were revealed, whether they thought they had been on placebo or active drug.
- Some of the spinal fluid markers that improved related to neuro-inflammation.That, and the improvement in the NDD-related markers, would not have been directly caused by a placebo effect. However, the increased mobility resulting from a placebo effect might have reduced neuro-inflammation, reducing in turn the markers of brain tissue damage. (Only the patients with PD, not AD, received testing for physical mobility and there was no record of the patients’ exercise habits.)
- Like many drug trials at this early stage, this one was not only sponsored by the drug company, but the first and last authors were company employees. I found no evidence of dishonesty in reading the paper, but a potential financial and professional conflict-of-interest does exist.
- As stated, this trial was only 25 days long, and we really need to know the longer-term side effects of depriving the brain of a whole raft of normal proteins, even if some of those molecules later cause mischief.
Enough for now. My next post will discuss the results of a larger, more recent trial of buntanetap that has not yet been published in a peer-reviewed journal. Cliffhanger.