A paper of mine just hit the streets today. Actually, the idea and most of the work came from an old friend and colleague at the University of Chicago, Dr. Tao Xie. (His last name is somewhere between “she” and “chee” and his first name is perfect for a PSP researcher.) Here’s the story of that project, from the beginning.
From 1994 to my retirement from practice in 2020, I kept a careful record of the PSP Rating Scale (PSPRS) results in all 526 patients I saw with PSP. The database includes each patient’s sex, birth year, month/year of PSP symptom onset, and death month/year (if deceased). For each visit, I recorded the month/year and each of the 28 PSP Rating Scale item scores. Back in 2020, some other colleagues and I published a paper on how to use the raw PSPRS scores to help predict prognosis in individual patients.
Tao asked if he could use my database, with my formal collaboration, to find a better way of predicting long-term survival. He said he didn’t just want to look at raw scores – he wanted to look at their magnitude and rate of progression at one critical point: the time when the person first developed difficulty looking down. That’s easily approximated by finding the date of the visit when the score on the PSPRS item for downgaze first exceeded zero. He would then correlate those “input variables” with, as “output variable,” the patient’s overall survival. The progression rate would be calculated as the raw item score divided by the number of years since PSP onset. I said, “great idea.”
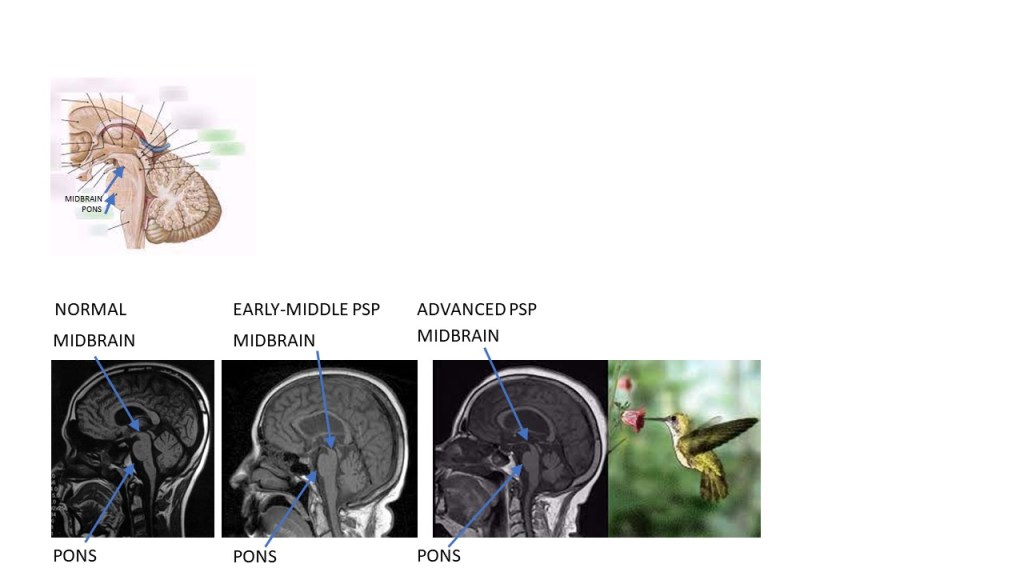
Why choose the onset of downgaze palsy as the benchmark? That’s when the insidious pathological process of PSP has first broken out of its three places of origin in the brain: the substantia nigra, the subthalamic nucleus and the globus pallidus. Why it starts in those three places is a mystery, but from there the abnormally folded tau protein molecules travel along the axons to other places, and pretty much their first stop is the area where downgaze is controlled, in the dorsal midbrain. (Perhaps relevantly, downgaze palsy is by far the most “specific” feature of PSP, meaning that of all of the disease’s features, that’s the one shared with fewest other diseases.)
So, Tao figured that once the process gets to the downgaze area, it has emerged from its birthplaces and is on its unfortunate way to other parts of the brain, probably at whatever speed is specified by the individual’s particular chemical and genetic makeup. Because that rate of transmission varies among individuals with PSP, it makes sense to measure the progression rate of PSP as of that stage of the disease rather than at a one-point-fits-all stage such as a set number of years after symptom onset.
Here’s what we found: The shorter survival is associated with older onset age and, as of the time of initial downgaze palsy, the PSPRS item scores for 1) difficulty swallowing liquids and 2) difficulty arising from a chair.
So, what does this mean? For care of an individual patient, the neurologist’s recommendations might be shaded to an extent by the knowledge that the patient’s future course will be more – or less – favorable than the published averages for PSP. In a large clinical trial, the statistician analyzing the data might want to achieve a more valid comparison of the active drug and placebo groups by weighting the progression data according to these factors.
Yes, research proceeds in small steps, but proceed it does.